Sleep impacts health and well being in many ways. This blog post addresses these impacts in two parts, with part I focused on specific health outcomes and part II focusing on the work-related impacts of poor or insufficient sleep for doctors.
Part I: Insufficient good quality sleep – increasingly recognized under the term “Insufficient Sleep Syndrome” (ISS), and recently identified as a possible major noncommunicable disease(1) – is associated with a wide range of significant health impacts:
- Cardiovascular Health:
- Increased risk of hypertension (2) – this is so real and so prevalent that, in this author’s opinion, sleep data should be queried in all patients on anti-hypertensive medications or in those creeping towards that need.
- Higher rates of cardiovascular disease(3), so much so that healthy sleep now stands alongside a healthy diet, regular exercise, and tobacco avoidance as a foundational pillar of heart health according to the American Heart Association(4)
- Metabolic Health:
- Greater likelihood of diabetes, insulin resistance, and obesity. There is so much data to support this (here’s a link to one scientist’s portfolio of work on the topic: https://www.salk.edu/
scientist/satchidananda-panda/ publications/).
- Greater likelihood of diabetes, insulin resistance, and obesity. There is so much data to support this (here’s a link to one scientist’s portfolio of work on the topic: https://www.salk.edu/
- Mental Health:
- Increased symptoms of anxiety, depression, and other mood disorders (5-7)
- Possible links to addiction and substance use disorders(8)
- Pain Perception:
- Higher acute pain sensitivity and increased pain scores (9)
- Headache Disorders:
- Higher risk of triggered migraines, potentially mediated by an accumulation of adenosine during sleep deprivation
- Accidents and Injuries:
- Increased risk of both fatal and non-fatal accidents (10,11)
- Immune Function:
- Potentially reduced vaccine efficacy(12,13)
- Neurological Health:
- Likely increased risk of dementia(14,15), potentially due to impaired clearance of beta-amyloid protein during sleep(16) and its accumulation during sleep deprivation(17)
- Cancer Risk:
- Higher risk of colon cancer(18)
- Mortality:
- Slightly increased all-cause mortality risk(19)
- Higher cancer-associated mortality rates for some cancers(20)
Note: Cancer studies often highlight a “Goldilocks zone” for sleep duration, with short and long sleep times both have been associated with increased mortality rates. However, this author has not seen any data that the latter is causal; rather, cancer can be associated with hyper-somnolence, and cancer progression may drive increased sleep time. The case for insufficient sleep and poor cancer outcomes seems more clear cut, and founded on data which implies a causal relationship.
Research on the impact of sleep insufficiency on fertility (and possibly on the outcomes of treatments for infertility) (21-23), and its connection to functionality in individuals with autism spectrum disorder (24,25), highlights the importance of assessing sleep quality. Prioritizing strategies to improve sleep may be an important component of care plans for these patients, although more research is needed in these domains.
Beyond the specific health impacts listed above, emotional processing, cognitive performance(26) including attention and focus, and stress management are all impacted by sleep. For the latter, high stress and poor sleep can be mutually reinforcing, setting up a negative feed forward cycle often called the sleep-stress cycle(27). The figure below provides a snapshot of the emotionally impacts of insufficient sleep.
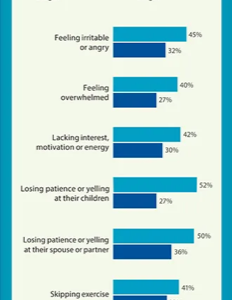
From the American Psychological Association’s, Stress in America™ 2013 survey (https://www.apa.org/news/
Finally, the discomfort caused by hyper-somnolence is not a medical condition in itself, but it can be a genuine source of suffering, comparable to pain from other causes. This symptom can significantly impact quality of life, much like any form of pain.
Part II: Beyond specific medical conditions, poor or insufficient sleep can affect doctors in other vital ways. Sleep impairment among healthcare workers is linked to several serious professional consequences, including increased risk of medical errors and reduced work performance. In one study (29), interns working traditional schedules with extended hours made more serious medical errors than those on schedules with reduced work hours. Further, these impacts were reversible: reducing the work hours of medical interns led to increased sleep and reduced attentional failures(28). Both studies, published over 20 years ago, provide evidence linking sleep deprivation with performance, including the occurrence of medical errors, among healthcare professionals. It’s time we pick up the conversation again, and make sleep protection a part of every physician training program.
Other aspects of work performance also are measurably impaired. Below is a clear and concise summary of this impact, quoted verbatim with full credit to the authors, and with their references included, from this highly important piece(30): “Emergency physicians working night shifts take longer to intubate,22 display an increased propensity for error as the shift progresses,23 and exhibit a significant decline in cognitive performance after working 5 consecutive night shifts.24 Sleep-impaired physicians in training exhibit deficiencies in functional cognition,25,26 concentration,
Finally, sleep-deprived doctors report significantly higher levels of burnout and reduced professional fulfillment(31). (Note: that study relied on subjective reports of sleep quality and sleepiness symptoms(32); while these scores have been correlated with total sleep time at least in one study(33), whether doctors – who have potentially endured years of sleep insufficiency – retain a reliable degree of subjective sensitivity to sleep deprivation is unclear). Multiple factors may contribute to a pro-burnout effect of sleep insufficiency. First, sleep deprivation can trigger a negative feedback loop of impaired cognitive performance, which in turn prolongs work hours as doctors struggle to complete their tasks, leading to more sleep insufficiency. Moreover, sleep deprivation hampers emotional processing which, if left unaddressed, can contribute to burnout. Here’s a plea worth heeding from a review that eloquently underscores the connection between sleep disruption and physician burnout: “Interventions should be directed not only at individuals but also at the entire health system”(34).
Thank you for tuning in, and here’s to good rest and good sleep for 2025 (and beyond)!
REFS:
- Chattu VK, Sakhamuri SM, Kumar R, Spence DW, BaHammam AS, Pandi-Perumal SR. Insufficient Sleep Syndrome: Is it time to classify it as a major noncommunicable disease? Sleep Sci. 2018;11(2):56-64. IPMID: 30083291
- Calhoun DA, Harding SM. Sleep and Hypertension. Chest. 2010;138(2):434-43. DOI: 10.1378/chest.09-2954
- Wang SS, Li ZX, Wang XY, Guo S, Sun YJ, Li GH, et al. Associations between sleep duration and cardiovascular diseases: A meta-review and meta-analysis of observational and Mendelian randomization studies. Frontiers in Cardiovascular Medicine. 2022;9. doi: 10.3389/fcvm.2022.930000
- Lloyd-Jones DM, Allen NB, Anderson CAM, Black T, Brewer LC, Foraker RE, et al. Life’s Essential 8: Updating and Enhancing the American Heart Association’s Construct of Cardiovascular Health: A Presidential Advisory From the American Heart Association. Circulation. 2022;146(5):E18-E43. https://www.ahajournals.org/
doi/10.1161/CIR. 0000000000001078 - Babson KA, Trainor CD, Feldner MT, Blumenthal H. A test of the effects of acute sleep deprivation on general and specific self-reported anxiety and depressive symptoms: An experimental extension. J Behav Ther Exp Psy. 2010;41(3):297-303. DOI: 10.1016/j.jbtep.2010.02.008
- Neckelmann D, Mykletun A, Dahl AA. Chronic insomnia as a risk factor for developing anxiety and depression. Sleep. 2007;30(7):873-80. DOI: 10.1093/sleep/30.7.873
- Weissman MM, Greenwald S, Nino-Murcia G, Dement WC. The morbidity of insomnia uncomplicated by psychiatric disorders. Gen Hosp Psychiatry. 1997;19(4):245-50. DOI: 10.1016/s0163-8343(97)00056-x
- Ostos-Valverde A, Herrera-Solis A, Ruiz-Contreras AE, Mendez-Diaz M, Prospero-Garcia OE. Sleep debt-induced anxiety and addiction to substances of abuse: A narrative review. Pharmacol Biochem Behav. 2024;245:173874. DOI: 10.1016/j.pbb.2024.173874
- Woelk J, Goerlitz D, Wachholtz A. I’m tired and it hurts! Sleep quality and acute pain response in a chronic pain population. Sleep Med. 2020;67:28-32. DOI: 10.1016/j.sleep.2019.10.017
- Garbarino S, Durando P, Guglielmi O, Dini G, Bersi F, Fornarino S, et al. Sleep Apnea, Sleep Debt and Daytime Sleepiness Are Independently Associated with Road Accidents. A Cross-Sectional Study on Truck Drivers. PLoS One. 2016;11(11):e0166262. DOI: 10.1371/journal.pone.0166262
- https://www.rospa.com/
getmedia/25999a67-6e67-4a8c- b32d-13b5c1090010/Driver- Fatigue-Factsheet-2022- updated.pdf - Spiegel K, Sheridan JF, Van Cauter E. Effect of sleep deprivation on response to immunization. JAMA. 2002;288(12):1471-2. DOI: 10.1001/jama.288.12.1469
- Spiegel K, Rey AE, Cheylus A, Ayling K, Benedict C, Lange T, et al. A meta-analysis of the associations between insufficient sleep duration and antibody response to vaccination. Curr Biol. 2023;33(5):998-1005 e2. DOI: 10.1016/j.cub.2023.02.017
- Robbins R, Quan SF, Weaver MD, Bormes G, Barger LK, Czeisler CA. Examining sleep deficiency and disturbance and their risk for incident dementia and all-cause mortality in older adults across 5 years in the United States. Aging (Albany NY). 2021;13(3):3254-68. DOI: 10.18632/aging.202591
- Sabia S, Fayosse A, Dumurgier J, van Hees VT, Paquet C, Sommerlad A, et al. Association of sleep duration in middle and old age with incidence of dementia. Nat Commun. 2021;12(1):2289. DOI: 10.1038/s41467-021-22354-2
- Nedergaard M, Goldman SA. Glymphatic failure as a final common pathway to dementia. Science. 2020;370(6512):50-6. https://pubmed.ncbi.nlm.nih.
gov/33004510/ - Shokri-Kojori E, Wang GJ, Wiers CE, Demiral SB, Guo M, Kim SW, et al. beta-Amyloid accumulation in the human brain after one night of sleep deprivation. Proc Natl Acad Sci U S A. 2018;115(17):4483-8. DOI: 10.1073/pnas.1721694115
- Chen J, Chen N, Huang T, Huang N, Zhuang Z, Liang H. Sleep pattern, healthy lifestyle and colorectal cancer incidence. Sci Rep. 2022;12(1):18317. DOI: 10.1038/s41598-022-21879-w
- Gallicchio L, Kalesan B. Sleep duration and mortality: a systematic review and meta-analysis. J Sleep Res. 2009;18(2):148-58. DOI: 10.1111/j.1365-2869.2008.
00732.x - Donzella SM, Deubler E, Patel AV, Phipps AI, Zhong C. Sleep and cancer mortality in the Cancer Prevention Study-II. Cancer Causes Control. 2024;35(12):1541-55. DOI: 10.1007/s10552-024-01910-3
- Zhao F, Hong X, Wang W, Wu J, Wang B. Effects of physical activity and sleep duration on fertility: A systematic review and meta-analysis based on prospective cohort studies. Front Public Health. 2022;10:1029469. https://pmc.ncbi.nlm.nih.gov/
articles/PMC9669984/ - Poster presentation / abstract: https://www.fertstert.org/
article/S0015-0282(17)30888-9/ fulltext - Info sheet from the University of North Carolina’s fertility center: https://uncfertility.com/
fertility-blog/the-link- between-sleep-and-fertility/ - Elkhatib Smidt SD, Gooneratne N, Brodkin ES, Bucan M, Mitchell JA. Sufficient sleep duration in autistic children and the role of physical activity. Autism. 2022;26(4):814-26. https://pmc.ncbi.nlm.nih.gov/
articles/PMC9010343/ - Devnani PA, Hegde AU. Autism and sleep disorders. J Pediatr Neurosci. 2015;10(4):304-7. https://pmc.ncbi.nlm.nih.gov/
articles/PMC4770638/ - Alhola P, Polo-Kantola P. Sleep deprivation: Impact on cognitive performance. Neuropsychiatr Dis Treat. 2007;3(5):553-67. PMID: 19300585
- Kalmbach DA, Anderson JR, Drake CL. The impact of stress on sleep: Pathogenic sleep reactivity as a vulnerability to insomnia and circadian disorders. J Sleep Res. 2018;27(6):e12710. PMID: 29797753
- Lockley SW, Cronin JW, Evans EE, Cade BE, Lee CJ, Landrigan CP, et al. Effect of reducing interns’ weekly work hours on sleep and attentional failures. N Engl J Med. 2004;351(18):1829-37. DOI: 10.1056/NEJMoa041404
- Landrigan CP, Rothschild JM, Cronin JW, Kaushal R, Burdick E, Katz JT, et al. Effect of reducing interns’ work hours on serious medical errors in intensive care units. N Engl J Med. 2004;351(18):1838-48. DOI: 10.1056/NEJMoa041406
- rockel MT, Menon NK, Rowe SG, Stewart MT, Smith R, Lu M, et al. Assessment of Physician Sleep and Wellness, Burnout, and Clinically Significant Medical Errors. JAMA Netw Open. 2020;3(12):e2028111 doi:10.1001/jamanetworkopen.
2020.28111 - Trockel MT, Menon NK, Rowe SG, Stewart MT, Smith R, Lu M, et al. Assessment of Physician Sleep and Wellness, Burnout, and Clinically Significant Medical Errors. JAMA Netw Open. 2020;3(12):e2028111 DOI: 10.1001/jamanetworkopen.2020.
28111 - Yu L, Buysse DJ, Germain A, Moul DE, Stover A, Dodds NE, et al. Development of short forms from the PROMIS sleep disturbance and Sleep-Related Impairment item banks. Behav Sleep Med. 2011;10(1):6-24. https://pubmed.ncbi.nlm.nih.
gov/22250775/ - Hanish AE, Lin-Dyken DC, Han JC. PROMIS Sleep Disturbance and Sleep-Related Impairment in Adolescents: Examining Psychometrics Using Self-Report and Actigraphy. Nurs Res. 2017;66(3):246-51. PMID: 28448375
- Stewart NH, Arora VM. The Impact of Sleep and Circadian Disorders on Physician Burnout. Chest. 2019;156(5):1022-30. DOI: 10.1016/j.chest.2019.07.008.
